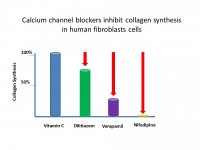
Popular High Blood Pressure Medicine Impairs Collagen Production In The Vascular Cells
The drugs intended to reduce blood pressure, correct arrhythmias and some forms of heart disease are the most commonly prescribed drugs in the US. One in every three adults, or approximately 75 million people, is diagnosed with high blood pressure in the US and many more have pre-hypertension. About 15 million people have some form of irregular heartbeats or arrhythmias. The most commonly prescribed drugs to treat these and other conditions are the so called “channel-blockers” or “agonists” which include calcium, sodium and potassium channel blockers. Worldwide sales of these drugs have reached $6 billion. In the United States, calcium channel blockers are the eighth largest drug class in prescription sales.
These drugs prevent calcium (and other valuable minerals) from entering the inside of the cells by blocking specific channels located in the walls of the smooth muscle cells lining the blood vessels, the cardiac muscle cells (myocytes) and other tissues. By blocking these channels the drugs cause relaxation of the cells and other pharmacological effects. Sodium transport channels are also used by Vitamin C to enter the cells.
A new study conducted at the Dr. Rath Research Institute and published in the American Journal of Cardiovascular Disease* shows that in addition to blocking the entry of calcium these drugs obstruct the uptake of vitamin C by the cells. Vitamin C is an essential nutrient for the production of collagen – the key stability molecule for blood vessel walls and connective tissue in general. Its long-term deficiency is especially detrimental for the cells building the artery walls as it can cause microscopic structural damage followed by the build-up of atherosclerotic deposits, the cause of heart attacks and strokes. The study indicates that among the studied channel blockers, nifedipine (i.e., Procardia, Nifediac) has the most pronounced effect causing a significant decrease of collagen production by the human vascular muscle cells. Taking into account that these drugs are supposed to be used for an indefinite time, their detrimental health consequences are of great concern.
In this aspect, the study shows that calcium-blocker-induced inhibition of collagen production by the cells can be compensated for by providing vitamin C. In particular, supplying fat-soluble vitamin C (ascorbyl palmitate), rather than simple vitamin C, resulted in significantly higher vitamin C concentration within the cells, further supporting collagen production.
The fact that calcium channel blockers – taken by tens of millions of heart patients worldwide in the belief that they can help prevent heart attacks – are actually increasing the risk for heart attacks due to weakening of the heart muscle and blood vessel walls, has been a major impediment in cardiology. In addition, increased risk of breast cancer and gum disease has also been reported. Based on the new study results it is possible that many of the side effects of these medicines could be prevented simply by supplementation of a synergistic combination of vitamin C, including ascorbyl palmitate, and other essential micronutrients.
* Ivanov V, et al., Am J Cardiovasc Dis 2016:6(2):26-35