Healthy Bones Need Healthy Connective Tissue
It is a popular perception that calcium and vitamin D are essential nutrients for healthy bones. However, few people are aware that bone health largely depends on its protein foundation – the collagen fibers. The alignment of collagen fibers within the bone (its “internal skeleton”) determine how calcium and other minerals are deposited, and therefore healthy collagen is the basis of the strength and stability of the entire bone.
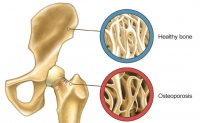
Osteoporosis - or thinning of the bones - is a disease where the bones lose density and strength which increases the risk of fractures and debilitation. Osteoporosis affects more than 200 million people worldwide. This figure includes both women and men over 50. Osteoporosis is the most common - yet least detected - bone metabolism disorder. In addition to a sedentary lifestyle, the use of prescription drugs such as corticosteroids, antacids such as proton pump inhibitors, and psychiatric medications, can cause excessive bone loss leading to osteoporosis. Although postmenopausal women are more likely to develop osteoporosis, one in five men will also develop significant bone thinning in their lifetime. In the elderly, thin bones are prone to breaking which can result in hip or vertebral fractures, and can increase the risk of premature death.
The formation of healthy collagen, which is the foundation for building strong bones, requires an optimum supply of essential micronutrients including vitamins C, D, and K2, the amino acids lysine and proline, and minerals such as calcium and many other micronutrients. Taking individual micronutrients such as vitamin D and calcium, even in mega doses, do not provide optimal bone health benefits. These two micronutrients need to be combined in synergistic proportions with others for enhanced efficacy.
At the Dr. Rath Research Institute, we investigated whether different combinations of micronutrients can affect the rate of bone thinning. We used female rats whose ovaries were removed to simulate the metabolic change observed in postmenopausal women (loss of estrogen production). One group of rats was given a specific combination of micronutrients, while the other group was left as the control group. In both groups we observed an accelerated bone thinning process; however, in the micronutrient supplemented group, the rate of bone formation dominated over bone resorption (thinning) when compared to the rats on a normal diet. The level of Gla-osteocalcin, which is an indicator of the mineralization of the bone, was also increased in the micronutrient supplemented group of animals. The serum calcium levels rapidly reduce when the ovaries stop functioning, such as during menopause; however, the micronutrient supplemented group of rats had normal serum calcium levels indicating they were restored due to supplementation.
Approximately half of all women start showing early signs of osteoporosis as young as 35-40 years of age. Since osteoporosis lacks specific symptoms, most patients are not diagnosed until extensive bone thinning has already set in. It is widely recommended to supplement with calcium and vitamin D for bone health. However, our study reiterates the importance of strong connective tissue, and utilizing a synergistic combination of micronutrients as a complete support of bone metabolism for maintaining a healthy and strong skeletal system over a lifetime.